Understanding Medicare Part B: What It Covers, What It Costs, and How to Enroll
Medicare Part B is the outpatient component of Original Medicare. While Part A handles hospital stays and inpatient care, Part B picks up the other half — doctor visits, lab work, preventive screenings, durable medical equipment, and a long list of outpatient services that most beneficiaries use far more frequently.
If you're approaching 65 or recently became eligible, understanding what Part B covers and what it costs is one of the most important steps in your Medicare journey. Skipping or delaying Part B enrollment can lead to permanent premium penalties that follow you for the rest of your time on Medicare.
What Does Medicare Part B Cover?
Part B covers medically necessary services — things your doctor orders to diagnose or treat a medical condition — along with a broad range of preventive services designed to catch problems early.
Doctor and Outpatient Services
- Doctor office visits — primary care and specialist appointments
- Outpatient surgery — procedures that don't require an overnight hospital stay
- Diagnostic tests — X-rays, MRIs, CT scans, blood work, and lab tests
- Mental health services — outpatient counseling, therapy sessions, and psychiatric visits
- Emergency room visits — the physician services portion (facility fees may fall under Part A)
- Ambulance services — when medically necessary
- Second opinions before surgery
Preventive Services
One of Part B's biggest advantages is its preventive care coverage. Most preventive services are covered at 100% with no cost-sharing when you see an accepting provider. These include:
- Annual wellness visit — a yearly check-in with your doctor to review your health and create a prevention plan
- Flu, pneumonia, COVID-19, and hepatitis B shots
- Cancer screenings — mammograms, colonoscopies, prostate exams, lung cancer screening
- Cardiovascular screenings — cholesterol, blood pressure, and heart disease risk checks
- Diabetes screenings and self-management training
- Depression screening
- "Welcome to Medicare" preventive visit — a one-time comprehensive physical within the first 12 months of enrollment
Durable Medical Equipment (DME)
Part B covers equipment prescribed by your doctor for home use:
- Wheelchairs and walkers
- Hospital beds
- Oxygen equipment
- Blood sugar monitors and testing supplies
- CPAP machines for sleep apnea
- Nebulizers
DME is covered at 80% of the Medicare-approved amount after your deductible — you pay the remaining 20%.
Other Part B Services
- Home health care — limited skilled nursing and therapy services at home
- Outpatient physical, occupational, and speech therapy
- Clinical research studies
- Kidney dialysis services and supplies
- Certain prescription drugs — Part B covers a small number of drugs administered by a doctor (such as chemotherapy infusions), while most prescriptions fall under Part D
What Does Medicare Part B Cost in 2026?
Part B has three cost components that every beneficiary should understand. For a complete look at all Medicare expenses, see our breakdown of how much Medicare costs in 2026.
Monthly Premium
The standard Part B premium for 2026 is $185.00 per month. This is deducted automatically from your Social Security check. Most people pay the standard amount, but higher earners pay more through the Income-Related Monthly Adjustment Amount (IRMAA).
IRMAA kicks in if your modified adjusted gross income (MAGI) from two years ago exceeds $106,000 for individuals or $212,000 for married couples filing jointly. At the highest income brackets, the Part B premium can be more than triple the standard amount.
Annual Deductible
The 2026 Part B deductible is $257. You pay this amount out of pocket before Part B starts covering its share. The deductible resets every calendar year.
Coinsurance
After meeting your deductible, you typically pay 20% of the Medicare-approved amount for most Part B services. There is no out-of-pocket maximum on Original Medicare — that 20% can add up quickly for expensive treatments, which is a key reason many people pair Part B with a Medicare Supplement plan.
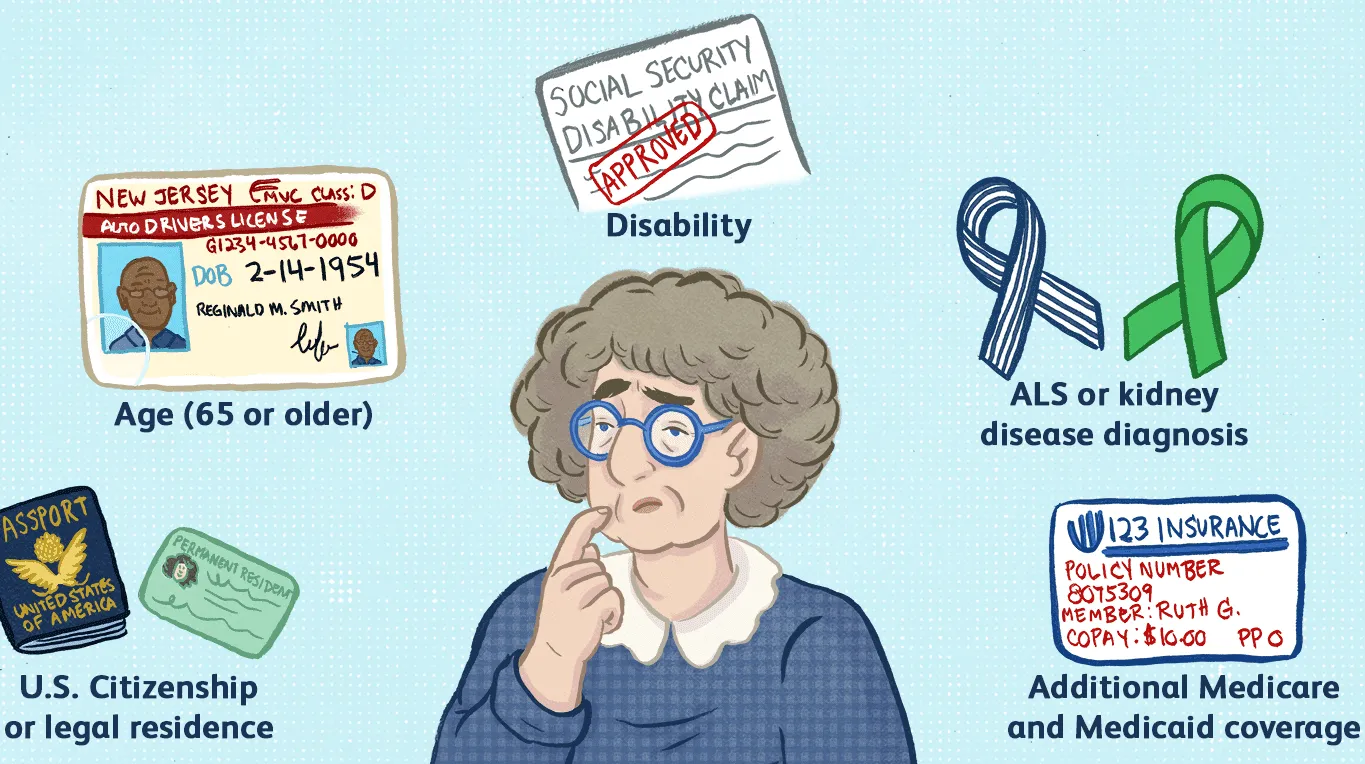
Who Is Eligible for Medicare Part B?
You're eligible for Part B if you meet any of the following criteria:
- Age 65 or older — you're a U.S. citizen or permanent resident who has lived in the U.S. for at least five consecutive years
- Under 65 with a qualifying disability — you've been receiving Social Security Disability Insurance (SSDI) for 24 months
- Any age with End-Stage Renal Disease (ESRD) — permanent kidney failure requiring dialysis or a transplant
- Any age with ALS — diagnosed with amyotrophic lateral sclerosis (Lou Gehrig's disease)
Eligibility for Part B does not depend on your work history. Even if you or your spouse never paid Medicare taxes, you can enroll in Part B — you'll just pay the full premium instead of the reduced rate most people get.
When to Enroll in Medicare Part B
Getting the timing right is critical. There are three main enrollment windows:
Initial Enrollment Period (IEP)
This is a seven-month window centered around your 65th birthday: three months before, your birthday month, and three months after. If you're turning 65 and don't have creditable employer coverage, this is when you should sign up.
General Enrollment Period (GEP)
If you missed your IEP, you can enroll during the General Enrollment Period from January 1 through March 31 each year. Coverage starts July 1. The catch: you'll likely face a late enrollment penalty.
Special Enrollment Period (SEP)
If you delayed Part B because you had coverage through an employer (or your spouse's employer) with 20 or more employees, you qualify for a Special Enrollment Period. You get eight months after the employment or group health coverage ends — whichever comes first — to sign up without a penalty.
This is one of the most misunderstood rules in Medicare. COBRA and retiree coverage do not count as employer coverage for this purpose. If you're relying on COBRA after leaving a job, sign up for Part B immediately — the SEP clock started when your employment ended, not when COBRA runs out.
The Part B Late Enrollment Penalty
If you don't sign up for Part B when you're first eligible and you don't have qualifying employer coverage, you'll pay a permanent premium surcharge. The penalty is 10% for each full 12-month period you could have had Part B but didn't.
For example, if you waited three years to enroll, your monthly premium would be 30% higher than the standard rate — for life. This penalty never goes away and compounds as the base premium increases each year. It's one of the costliest Medicare penalties you can face.
What Medicare Part B Does Not Cover
Understanding Part B's limits is just as important as knowing what it covers. Part B generally does not pay for:
- Most prescription drugs — you need a separate Part D plan or a Medicare Advantage plan with drug coverage
- Routine dental care — cleanings, fillings, dentures, and most dental work (learn more about whether Medicare covers dental)
- Routine vision care — eyeglasses, contacts, and routine eye exams (Part B does cover glaucoma screening and cataract surgery)
- Hearing aids — though Part B covers diagnostic hearing exams
- Long-term care — nursing home stays, assisted living, and custodial care
- Care outside the U.S. — with very limited exceptions
- Cosmetic surgery
Many of these gaps can be filled through Medicare Advantage plans, standalone Part D plans, or supplemental insurance.
Part B and Your Other Medicare Coverage
Part B doesn't exist in a vacuum — it's one piece of your overall Medicare picture:
- Original Medicare (Part A + Part B) — the foundation. Most people have premium-free Part A and pay the standard Part B premium. For details on what Part A costs separately, see our guide to Medicare Part A premiums and deductibles.
- Medicare Supplement (Medigap) — fills the gaps in Original Medicare, including Part B's 20% coinsurance and annual deductible. You must have both Part A and Part B to buy a Medigap plan.
- Medicare Advantage (Part C) — an alternative to Original Medicare that bundles Part A, Part B, and often Part D into one plan. You still pay your Part B premium, but the plan handles your cost-sharing differently — usually through copays and an out-of-pocket maximum.
- Part D — standalone prescription drug coverage. Needed if you have Original Medicare, since Part B only covers a handful of provider-administered drugs.
Tips for Getting the Most Out of Part B
- Schedule your Annual Wellness Visit every year. It's free and helps your doctor catch issues early.
- Know the difference between "observation" and "inpatient." If you're in the hospital under observation status, you're technically an outpatient — Part B covers the services, but the cost-sharing rules are different than a Part A inpatient stay.
- Ask if your provider accepts Medicare assignment. Providers who accept assignment agree to charge no more than the Medicare-approved amount. Those who don't can charge up to 15% more (called "excess charges").
- Consider a Medigap plan for the 20% coinsurance. Without supplemental coverage, one major procedure could leave you with a significant bill.
- Track your IRMAA. If your income drops due to a life-changing event (retirement, divorce, death of a spouse), you can request a redetermination to lower your premium.