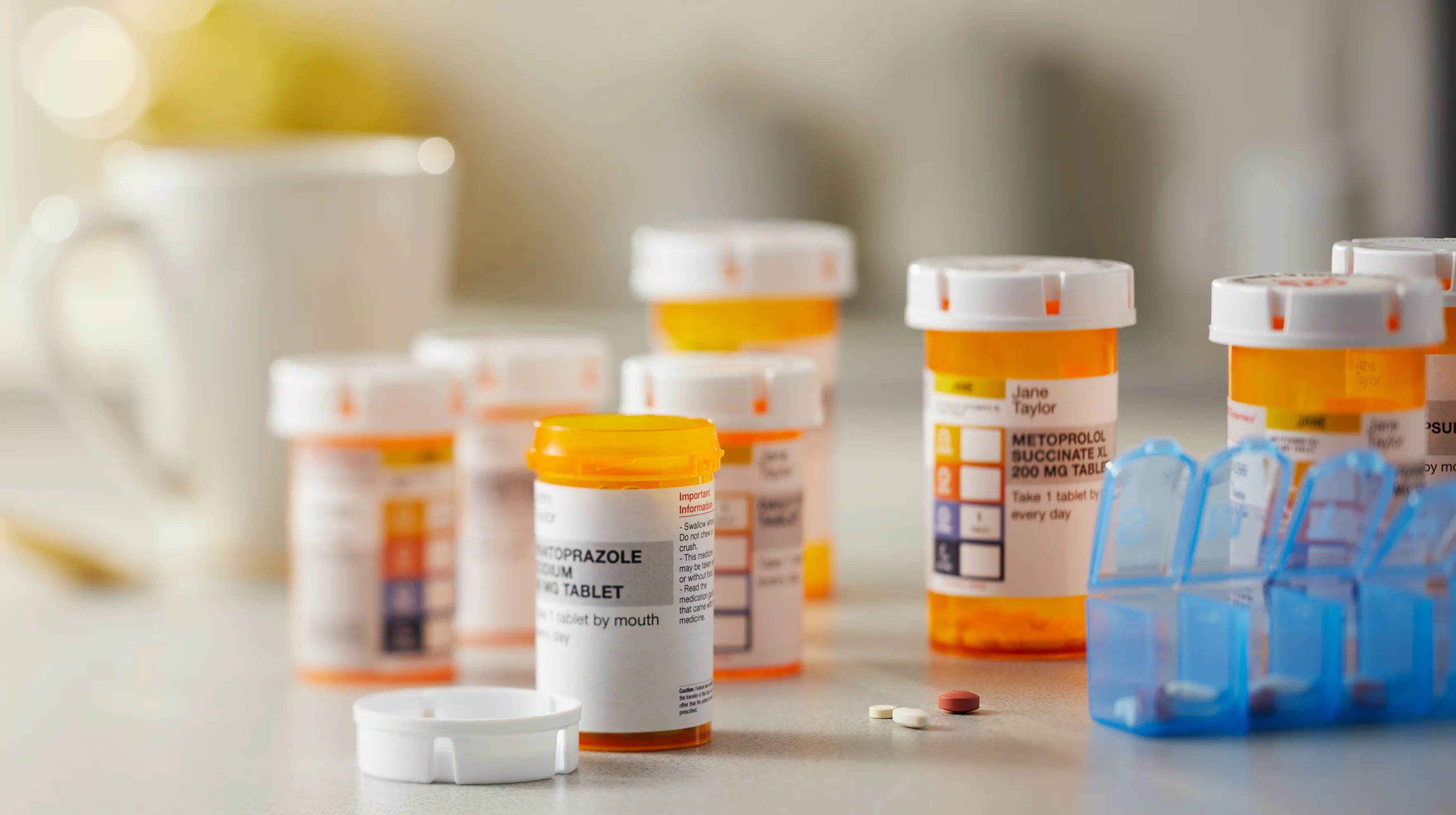
The $2,000 Medicare Part D Out-of-Pocket Cap: How It Works in 2026
If you take expensive prescription drugs, 2026 is the first full year you'll feel the biggest change to Medicare Part D in two decades: a hard $2,000 cap on your annual out-of-pocket drug spending. Once you hit that cap, your Part D plan pays 100% of covered drug costs for the rest of the calendar year.
This single change replaces the old "donut hole" math that often left beneficiaries on the hook for thousands of dollars before catastrophic coverage kicked in. Here's exactly how the new cap works, who benefits most, and the lesser-known monthly payment option that goes with it.
What Changed Under the Inflation Reduction Act
The Inflation Reduction Act rewrote the financial structure of Part D in stages. Two dates matter:
- January 1, 2025 — the $2,000 annual out-of-pocket maximum took effect for the first time.
- January 1, 2026 — the cap indexes upward with Part D spending growth and the Medicare Prescription Payment Plan is now a mature, plan-year-one-tested option.
The old coverage gap (the "donut hole") is gone in the way most people remember it. You can read the background in our guide to the Medicare donut hole and how the coverage gap worked, but the short version is: once your true out-of-pocket spending on covered drugs hits $2,000, you pay $0 for the rest of the year.
How the $2,000 Cap Actually Works
Part D now has three simplified phases instead of four:
- Deductible phase — you pay 100% of drug costs up to your plan's deductible (maximum $615 in 2026; many plans set it lower or at $0 for generics).
- Initial coverage phase — you pay a copay or coinsurance (often 25%) and the plan pays the rest until your out-of-pocket spending hits $2,000.
- Catastrophic phase — once you hit $2,000, you pay nothing for covered Part D drugs for the rest of the year.
What counts toward the $2,000? Your deductible, copays, and coinsurance on covered drugs. Premiums do not count. Drugs that your plan doesn't cover — or that you buy outside your plan — also don't count.
Who Benefits the Most
The cap helps everyone with Part D, but the savings are dramatic for a specific group: people on high-cost specialty medications. Before 2025, a single month of a cancer drug, MS therapy, or advanced biologic could cost thousands out of pocket. Today, your total yearly cost for covered drugs is capped — period.
You benefit the most if you:
- Take a brand-name drug with no generic equivalent
- Take multiple maintenance drugs that together push you past $2,000
- Are on a specialty tier medication (cancer, autoimmune, rare disease, etc.)
- Previously hit the catastrophic phase and still paid 5% of drug costs
If you previously spent $500 or less per year on prescriptions, your day-to-day experience won't change much — but the protection is there if your health situation changes.
The Medicare Prescription Payment Plan (M3P)
The cap comes with a quiet but powerful companion feature: the Medicare Prescription Payment Plan, sometimes called M3P or "smoothing."
Here's the problem it solves: even with a $2,000 cap, you could still owe $2,000 in January if your plan has a deductible and you fill an expensive prescription early in the year. That lump-sum shock is real, especially on a fixed income.
M3P lets you spread your Part D out-of-pocket costs across the remaining months of the year in predictable monthly bills from your plan. You pay $0 at the pharmacy counter; your plan bills you monthly instead.
Key things to know about M3P:
- It's optional and free — there's no fee to participate.
- You can opt in before the plan year starts or at any point during the year.
- You don't save money — you pay the same total amount — but you avoid pharmacy-counter shock.
- If you miss a monthly bill, you can be removed from the program, though your drug coverage itself continues.
M3P is most valuable for people whose drug costs are front-loaded in the year, or who simply budget better with predictable monthly bills. It's less helpful if your drug costs are modest and spread evenly across the year.
How the Cap Changes Plan Selection
With a hard $2,000 ceiling, the math for choosing a Part D plan is different than it was even two years ago. A few principles:
Formulary still matters more than anything. If your drug isn't on a plan's formulary, the $2,000 cap does nothing for you — you'll pay full price out of pocket and it won't count toward the cap. Always check the formulary for every drug you take.
Premiums matter more, relatively. When out-of-pocket costs are capped, the premium becomes a bigger share of your total annual spend. A plan with a $40 monthly premium costs you $480 a year whether you use it or not.
Pharmacy network matters. Preferred pharmacies still offer lower copays, which means you hit the $2,000 cap later (or not at all) — keeping more money in your pocket if your drug costs are modest.
Our guide to comparing and choosing a Medicare Part D plan walks through these trade-offs in detail. And if you've missed an enrollment window, review our breakdown of the Part D late enrollment penalty before assuming you can wait.
Common Questions
Does the cap apply to Medicare Advantage drug coverage (MA-PD) too?
Yes. If your Medicare Advantage plan includes Part D drug coverage, the $2,000 cap applies to the drug portion of your costs.
Do manufacturer coupons count toward the cap?
No. Only what you actually pay out of pocket for covered Part D drugs counts. Manufacturer assistance can still help you pay, but it doesn't accelerate hitting the cap.
What if I qualify for Extra Help or a Medicare Savings Program?
You're likely already paying far less than $2,000 a year. The new cap is an added backstop, but the bigger savings come from the low-income subsidy programs — see our overview of Medicare Savings Programs and how to get help paying for Medicare costs.
Does the cap reset each year?
Yes. It's a calendar-year cap. Every January 1, the meter resets to $0.
What to Do Before Your Next Enrollment Period
- List every prescription you take, including dosage and quantity.
- Run each one through the Medicare Plan Finder at Medicare.gov — it will estimate your yearly out-of-pocket cost by plan.
- Check whether any plan hits the $2,000 cap faster based on your specific drug mix.
- Decide if M3P makes sense for your budget — especially if you start the year with a pricey refill.
- Talk to a licensed agent if your drug list is complex. A local agent who specializes in Part D can often spot savings you'd miss on your own — see why working with a local insurance agent pays off.
The $2,000 cap is the biggest piece of financial protection Medicare beneficiaries have gained in a generation. Understanding how it fits together with your plan's formulary, premium, and pharmacy network is the difference between merely having the protection and actually getting the most out of it.