Understanding Medicare Part A: Insurance Coverage for Hospital Related Services
What Is Medicare Part A?
Medicare Part A is the portion of Original Medicare that covers inpatient hospital care, skilled nursing facility stays, hospice care, and some home health services. Most people get Part A automatically and pay no monthly premium if they or their spouse paid Medicare taxes for at least 40 quarters (10 years) while working.
Who Is Eligible for Medicare Part A?
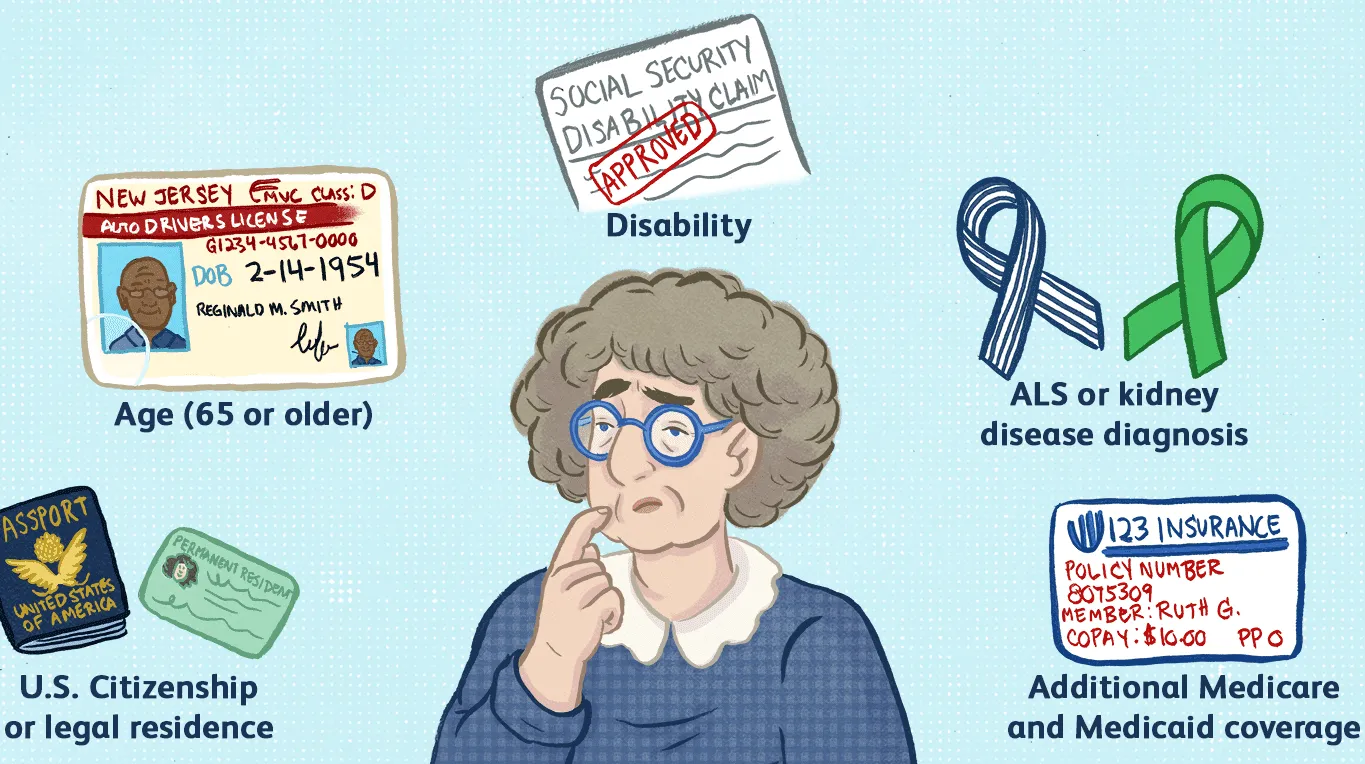
Eligibility for Medicare Part A is automatic for most people when they turn 65 and are already receiving Social Security or Railroad Retirement Board benefits. You may also qualify for Medicare before age 65 if you:
- Have received Social Security Disability Insurance (SSDI) for 24 months
- Have been diagnosed with End-Stage Renal Disease (ESRD)
- Have been diagnosed with Amyotrophic Lateral Sclerosis (ALS)
You must also be a U.S. citizen or a legal permanent resident who has lived in the United States for at least five consecutive years.
What Does Medicare Part A Cover?
Part A covers medically necessary inpatient care across several settings:
- Inpatient hospital care — semi-private room, meals, nursing services, medications, lab tests, and other supplies provided during your stay
- Skilled nursing facility (SNF) care — up to 100 days per benefit period following a qualifying hospital stay (custodial-only care is not covered)
- Home health services — intermittent skilled nursing care and therapy services when you’re homebound
- Hospice care — comfort care for terminally ill beneficiaries, including medication for symptom management
- Inpatient psychiatric care — up to 190 days lifetime in a psychiatric hospital
What Part A Does Not Cover
Medicare Part A does not cover:
- Private hospital rooms (unless medically necessary)
- Private-duty nursing
- Personal comfort items (phone, TV, toiletries)
- The first three pints of blood (unless donated to the hospital)
- Long-term custodial care (assisted living, most nursing home stays)
2026 Medicare Part A Costs
Understanding what you’ll pay is critical for planning your healthcare budget. For a detailed breakdown, see our guide to Medicare Part A costs, premiums, and deductibles in 2026. Here are the current 2026 Part A costs:
Monthly Premiums
Most beneficiaries pay $0 per month for Part A if they or their spouse paid Medicare taxes for 40+ quarters. If not:
- 30–39 quarters of Medicare tax payments: $311 per month
- Fewer than 30 quarters: $565 per month
Deductible and Coinsurance
Part A uses a benefit period structure rather than an annual deductible. Each time you’re admitted to the hospital, a new benefit period may begin (a benefit period ends when you’ve been out of the hospital or SNF for 60 consecutive days).
- Deductible: $1,736 per benefit period
- Days 1–60: $0 coinsurance (after deductible)
- Days 61–90: $434 per day coinsurance
- Days 91+: $868 per day using lifetime reserve days (you get 60 lifetime reserve days total)
- Skilled nursing facility days 21–100: $217 per day coinsurance
Part A costs are just one piece of the total cost of Medicare in 2026, which also includes Part B premiums, drug plan costs, and supplemental coverage.
How to Enroll in Medicare Part A
If you’re already receiving Social Security benefits, you’ll be automatically enrolled in Part A when you turn 65. If you’re not receiving Social Security, you’ll need to actively enroll in Medicare during your Initial Enrollment Period — a seven-month window that starts three months before your 65th birthday month.
If you miss your Initial Enrollment Period, you can sign up during the General Enrollment Period (January 1 – March 31 each year), with coverage starting July 1. Late enrollment may result in premium penalties if you didn’t have qualifying coverage. Stay informed about upcoming changes to Medicare that may affect enrollment rules and costs.
How to Pay Your Part A Premium
If you do owe a monthly premium, Medicare offers four payment methods:
- Online — pay by credit or debit card through your Medicare account
- Direct bank payment — pay from your savings or checking account
- Medicare Easy Pay — free automatic monthly deduction from your bank account
- Mail — send a check to Medicare
Protecting Yourself Beyond Part A
While Part A covers a significant portion of inpatient costs, the deductibles and coinsurance can add up fast — especially during extended hospital stays. Many beneficiaries pair Part A with a Medicare Supplement (Medigap) plan to help cover these out-of-pocket expenses. Others choose a Medicare Advantage plan that bundles Part A, Part B, and often Part D into a single plan with different cost-sharing rules.